Tues: 8:30am - 3:00pm
Wed: 12:00pm - 6:00pm
Thurs: 8:30am - 3:00pm
Fri: Closed
Sat: 8:30am - 12:30pm
Sun: Closed
Greenvale, NY 11548
Managing Melasma
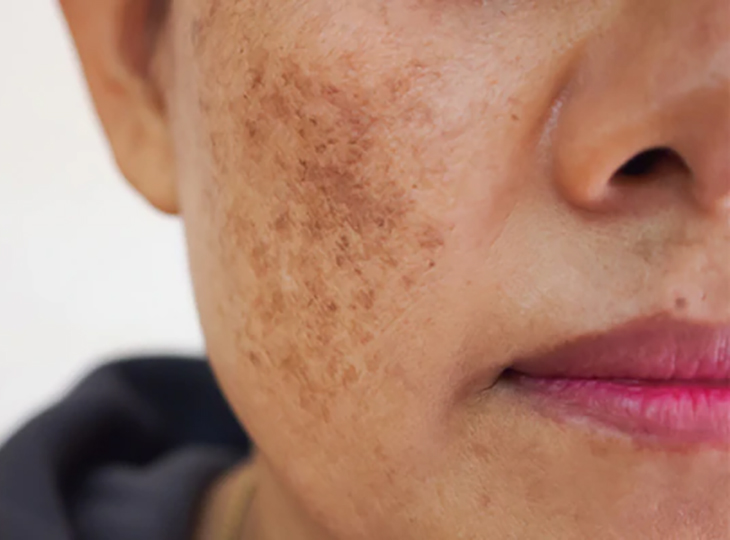

Melasma is a skin condition that causes dark patches and spots, usually on the face. The word means “black spot.” While common, to the untrained eye melasma can be mistaken for other skin conditions. A dermatologist can give you an accurate diagnosis and prepare a treatment plan. The skin condition is more common among Latinos and women, according to the American Academy of Dermatology. About 90% of people who get melasma are women.
Melasma is not skin cancer nor is it a sign of cancer. Although not dangerous, melasma has been shown to have a significant emotional and psychologic effect on patients, who are usually women. This pigmentary disorder also appears to be more prevalent among Latinos, according to the National Institutes of Health. Skin pigmentation appears to be the most likely reason.
Your dermatologist knows that treating melasma in darker skin tones requires a different approach. Some melasma treatments can actually irritate darker skin, which can worsen melasma. This is why seeing a dermatologist is advisable before you attempt home remedies or over-the-counter treatments.
It’s important to know that no matter your skin tone, melasma can be a stubborn skin condition. Some patients will require a prescription-strength cream or other treatment. If you suspect you have melasma, fear not. It’s a common skin disorder, especially among pregnant women. Up to 50% of women will develop this condition during a pregnancy, according to the Cleveland Clinic. The rate is higher among Latina women. Up to a third of the population may get melasma — and it happens more often during a woman’s reproductive years, though rarely during puberty. It usually starts between 20 and 40 years of age.
What causes melasma?
Your epidermis contains cells called melanocytes that store and produce a dark pigment known as melanin. When exposed to light, heat, ultraviolet radiation or through hormonal stimulation, the melanocytes produce more melanin. The result is darker skin. Melasma occurs when melanin darkens in patches or spots on the skin. Melasma can be triggered by a variety of causes. These are the most common:
- Internal factors such as genetics (family history), having naturally darker skin, and hormone changes. The skin pigmentation of Latino women and men appears to be more susceptible to melasma.
- External factors, including UV light exposure (especially prolonged sun exposure and working outdoors), skin inflammation, irritation from certain skin-care products, some medications, and oral contraceptives.
- Pregnancy can also trigger the condition; melasma is known as the “mask of pregnancy.” Hormonal changes during pregnancy are the likely cause.
Melasma can also affect men. Sun exposure and working outdoors are the major risk factors for men.
The clinical presentation of melasma is similar in men and women, with dark brown patches and macules (spots that resemble freckles), which develop on the face, neck, shoulders and upper arms.
Again, while not dangerous, the appearance of melasma can be a source of embarrassment, as it affects our appearance. There is no cure for melasma, but it can be treated and in some cases goes away on its own. If you dislike the discoloration on your skin caused by melasma certain treatments can help. Dermatologists recommend treating melasma sooner rather than later. It can be difficult to get good results from treatment if you’ve had melasma for years.
Why do women get melasma when they’re pregnant?
Pregnant women get melasma more often than anyone else. You’re also at risk if you take oral contraceptives and hormones. Pregnant women also have increased levels of the hormones estrogen and progesterone. These hormones are thought to contribute to melasma. The darker color usually fades after pregnancy.
Important note: If you are pregnant, wait until your baby is born before treating melasma. Some treatments that you can buy without a prescription may be labeled as harmful for use during pregnancy. Melasma may even improve and perhaps go away after you give birth.
Other leading causes of melasma may include:
- Tanning beds. UV light produced by tanning beds damages your skin as badly as the sun’s radiation and may even be worse.
- Antiseizure drugs.
- Birth control pills. Melasma has been identified in individuals who use oral contraceptive pills that contain estrogen and progesterone.
- LED Screens – the light from your laptop, cell phone, tablet and most television sets.
- Estrogen/Diethylstilbestrol, which is a man-made form of the hormone estrogen. It’s commonly used in prostate cancer treatment.
- An underactive thyroid.
- Makeup. Some cosmetics can cause a phototoxic reaction that triggers melasma.
- Phototoxic drugs. These are medicines that make you sensitive to sunlight and include some antibiotics, nonsteroidal anti-inflammatory drugs, diuretics, retinoids, hypoglycaemics, antipsychotics, and other drugs. You’ll want to share a list with your dermatologist of any medications you take.
- Any product that irritates the skin will probably worsen your melasma.
- Research shows some scented soaps may cause or worsen the condition.
What are my melasma treatment options?
Melasma is not a harmful condition and some individuals may decide not to seek treatment. However, studies have shown that melasma can negatively impact an individual’s quality of life both socially and professionally. The appearance of melasma can make people feel more self-conscious. Melasma is a manageable skin condition, so seeking treatment early can help reduce the appearance of dark patches as well as prevent them from coming back. There are many types of treatment:
- Topical creams: These medications are applied directly to the skin and are designed to reduce melanin production, encourage new skin growth, and lower inflammation.
- Chemical peels: A solution applied by either an aesthetician or dermatologist, which then peels off the topmost skin layer, removing discolored patches and encouraging new skin growth.
- Laser skin lightening: Your aesthetician or dermatologist uses a precision laser to remove discolored areas.
- Oral treatments: Prescription medications that slow melanin production and lighten the characteristic dark patches on the skin.
- Microneedling: A procedure using small needles to help topical melasma creams penetrate more deeply into the skin, leading to improvement in the appearance.
- Microdermabrasion: Friction-based tools to exfoliate the skin, help cell turnover and promote new skin growth.
- Home remedies. These include topical applications of apple cider vinegar, essential oils, turmeric, and others. These treatments have not been scientifically evaluated and should only be used following a consultation with your dermatologist.
Any treatment plan should include sun protection because UV rays can make melasma worse. If you have discolored patches or freckle-like spots on your skin, seeing a dermatologist can reduce your worries. A dermatologist can tell you whether melasma or another condition is causing the discoloration.
If you have melasma, a dermatologist can also develop an individualized treatment plan for you. Treatment usually begins with sun protection and creams that you apply to the skin over the affected area.
Many people who have a darker skin tone, Latinos especially, see a dermatologist for melasma treatment. Melasma is actually one of the most common reasons that people who have darker skin see a dermatologist. While it is unclear why melasma disproportionately affects Latinos, a higher concentration of melanin and related genetics are most likely contributing factors.
Is melasma permanent?
Only in the rarest cases. Melasma is commonly a chronic disorder. This means that it typically lasts three months or more, then fades away. However, some people have melasma for years or their entire lives. Other people may have melasma for only a few months, such as during pregnancy.
Let Walk-in Dermatology Take Care of You
If you have concerns about melasma or any skin condition and need dependable answers you don’t have to wonder, worry or wait. Walk-in Dermatology is here to keep you healthy. Our team of dermatologists and experienced healthcare staff will address your concerns and provide the necessary care for all your skin conditions. We can set up a Video Visit and even prescribe medications remotely, or you can schedule an appointment with us online. The choice is yours. But don’t wait until the problem gets worse. Contact us today.