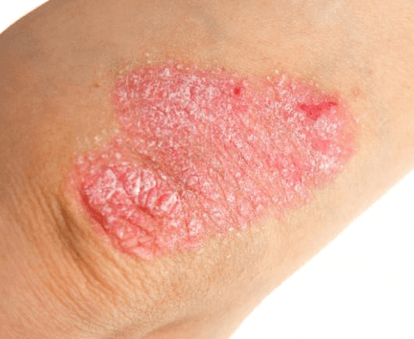
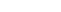Psoriasis is a chronic, autoimmune condition that causes skin cells to multiply faster than normal. The skin begins to form into red patches with white scales and bumps. Psoriasis is most common on the scalp, elbows, knees and lower back, although it can form anywhere on the body. Plaque psoriasis, which is the most common type, causes dry, red skin bumps and thick lesions (plaques) with white or silver-colored scales. Psoriasis is often itchy and sometimes painful. There are several types of psoriasis including plaque psoriasis, guttate psoriasis, inverse psoriasis, and pustular psoriasis.
Tues: 8:30am - 3:00pm
Wed: 12:00pm - 6:00pm
Thurs: 8:30am - 3:00pm
Fri: Closed
Sat: 8:30am - 12:30pm
Sun: Closed
Greenvale, NY 11548
Psoriasis

What is psoriasis?
Psoriasis is not contagious. You cannot “catch” this condition from another person.
Why does psoriasis occur?
While the exact cause is not yet known, research shows that the cause of psoriasis is related to a combination of a persons’s genes and their body’s immune system. In patients with psoriasis, the white cells of the immune system, known as T-cells, in addition to doing their job of attacking viruses and bacteria, start attacking the body’s skin cells. This triggers areas of skin to make more skin cells more quickly, resulting in piling up of skin cells on the body and what clinically presents as the plaques of psoriasis.
How dermatologists diagnose psoriasis
Your dermatologist will determine the diagnosis and extent of your psoriasis by reviewing your medical history (including history of joint pain) and conducting a thorough physical exam that consists of examining your skin, scalp and nails. In some cases, it may be necessary to take a small skin sample, known as a biopsy, to diagnose the condition.
How dermatologists treat psoriasis
Treatment of psoriasis is based on several factors including type of psoriasis, location of skin lesions, severity of psoriasis (including body surface area affected), impact of condition on daily life, joint involvement, and other medical conditions you have.
Psoriasis is most commonly treated with the application of topical creams and ointments on the skin. These topical medications include corticosteroids, synthetic vitamin D, retinoids, and calcineurin inhibitors (tacrolimus ointment and pimecrolimus cream).
If the psoriasis is severe or debilitating or not controlled with topical treatments, a dermatologist may discuss prescribing oral medications or injectable treatment, known as biologic therapy.
Light therapy is another option where the skin is exposed to natural sunlight or artificial ultraviolet light for set periods.
Oral medications used to treat psoriasis include Otezla and cyclosproine, which are both taken in pill form. Before prescribing these medications, your dermatologist will need to review your personal/family medical history, other medicines you take, and whether there is a history of kidney disease in your family. Medical tests prior to taking this drug and during treatment include blood testing.
Biologic therapy is prescribed when other treatments have not been effective in controlling the symptoms of psoriasis and/or psoriatic arthritis. Biologics were developed to calm the immune system that is overactive in psoriasis. They are given as injections at specific time intervals. There are several different biologic treatments that have been FDA approved to treat psoriasis. While biologics are very effective in treating psoriasis, there are serious side effects that can develop while taking them including infections. It is important to discuss the risks and benefits of these medications with your dermatologist when deciding on what treatment option is best for you.